Key points:
- The healthcare and social assistance subsectors played a key role in driving aggregate employment growth in 2025, and now make up about 15% of the US workforce.
- The ability of these subsectors to offset an otherwise slowing labor market will likely depend on the extent to which they can absorb workers from other industries.
- Healthcare occupations tend to have higher barriers to entry, such as licensing requirements, making it harder for workers to switch into the expanding sector. Additionally, job postings by healthcare companies for non-healthcare roles have slowed.
- Compared to 2022, a greater share of healthcare job postings are concentrated in companies that specialize in the field.
As hiring slowed in 2025, the healthcare and social assistance subsectors became increasingly important drivers of aggregate job gains, adding 690,000 jobs nationwide, even as many other sectors shed jobs at levels typically seen during recessions. Overall employment in healthcare and social assistance fields has been growing strongly since the Great Recession, and the sector currently employs around 15% of the US workforce.
This shift in concentration raises important questions: Is it a problem if too many people work in a single sector? How many workers can these industries absorb? And is this sustainable in an otherwise slowing labor market?
Healthcare and social assistance’s long climb
Driven by factors including rising incomes, expanding access to health insurance, medical product innovation, and longer life expectancies, the healthcare and social assistance subsector has been steadily increasing as a share of the labor force for over 30 years. As the largest waves of Baby Boomers have begun to reach retirement age, these dynamics have intensified. For example, demand for home healthcare workers has grown considerably and is expected to continue to increase steadily in the coming years. But while this particular segment has been growing for decades, its more recent rise in the post-pandemic period has been particularly notable. Since hitting its post-pandemic low in March 2022, healthcare and social assistance employment has grown at close to twice the pace it did between 2010 and early 2020.
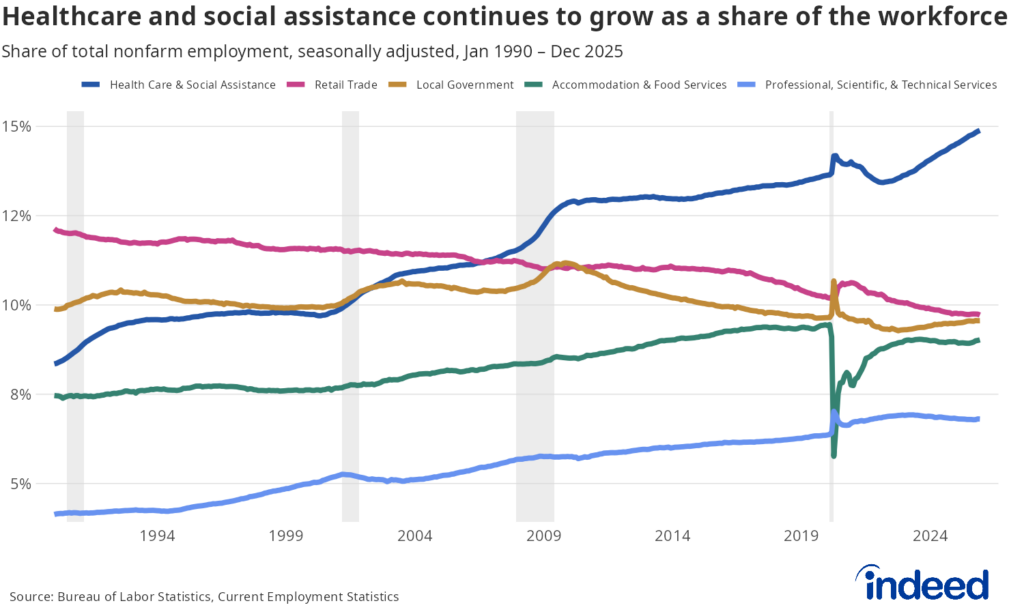
Line graph titled “Healthcare and social assistance continues to grow as a share of the workforce” shows the share of jobs that healthcare workers have made up of the labor force since 1990.
Hospitals and physicians’ offices have played an important role in this growth, with overall employment in these areas increasing by 2.1% and 2.4%, respectively, in 2025 compared to 2024. That said, the strongest growth in the subsector is coming from areas outside what might be considered traditional healthcare services. Employment in individual and family services —part of the social assistance side of the sector — grew by 8.8% year-over-year in 2025, more than double the pace of the next fastest-growing subsector. The individual and family services segment primarily includes non-residential social assistance roles focused on children, families, older adults, and individuals with disabilities, with nursing aides, patient aides, and social workers among the most common job titles.
Can healthcare and social assistance reinforce a slowing labor market?
Because it is often a matter of medical necessity and paid for through insurance or other means, demand for healthcare services is generally less sensitive to broader economic conditions. For this reason, when the economy slows, companies in these sectors are usually able to absorb some amount of displaced workers. During the Great Recession, for example, healthcare and social assistance’s share of the workforce grew substantially while similarly sized sectors fell or held flat.
At the same time, many of the unique requirements of healthcare and social assistance roles can complicate a transition into the sector for people with experience in other industries or roles. Specific educational requirements, credentials, or licensures are disproportionately required across many healthcare roles, which can increase barriers for workers aiming to switch from other sectors.
Indeed data indicate that 6 of the 10 occupational sectors most likely to require professional licensure are commonly associated with the healthcare and social assistance subsector (including nursing, therapy, and dental work). Specific healthcare certifications are sometimes required for many non-healthcare-related roles; a public safety officer may need a first-aid certification, or a maintenance technician may need special certification to work on complex medical equipment. But in general, the share of jobs requiring specific medical certifications or training is much higher in occupations that are commonly found in the healthcare and social assistance subsector. For example, about 92% of all nursing roles require some certification, with 90% requiring specific medical certifications, while 55% of installation and maintenance roles require some certification, with just 0.4% requiring specific medical certification.
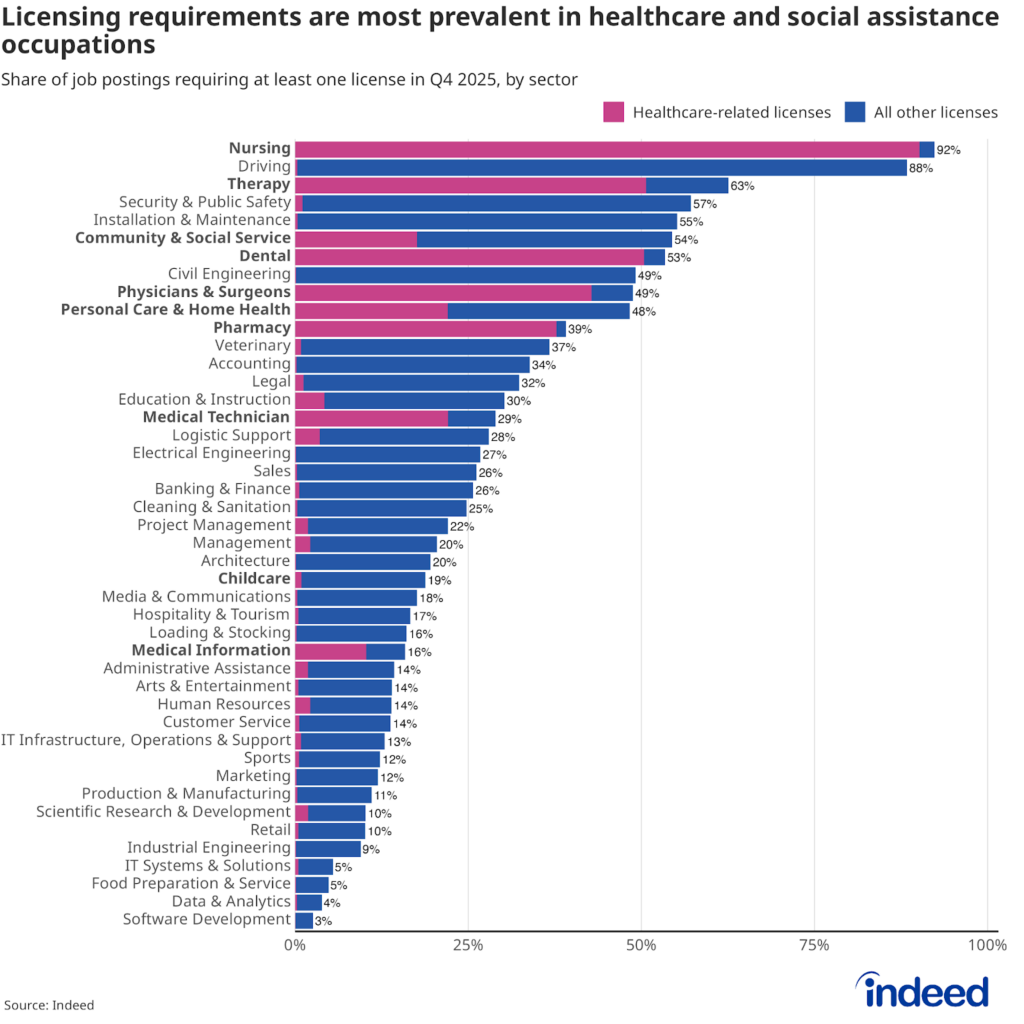
These licensing requirements act as barriers to entry into what is, essentially, the only sector currently seeing a meaningful rise in payroll employment. This is especially true for healthcare licensures, which typically require some level of postsecondary education. For example, although the administrative assistance and medical information occupational sectors involve jobs that perform similar tasks, licensing requirements differ substantially. Medical information roles — including medical billers, patient service representatives, and medical office assistants — are about eight percentage points more likely to require a healthcare-related license than administrative assistance roles. This higher licensing burden may limit workers’ ability to transition seamlessly into the healthcare and social assistance subsector.
It’s important to note that Indeed’s data only indicates the share of job postings that explicitly list licensing requirements, and it’s common for job postings in some sectors to leave out obvious, expected licensing requirements. For example, all physicians must possess a valid medical license issued by the medical board in the state or jurisdiction where they practice. However, not all job postings for physicians & surgeons explicitly state that these licenses are required, since it may be logically implied or assumed. As a result, job postings data will always underestimate the actual licensure requirements and, consequently, the barriers to entry in these fields.
Non-healthcare roles in healthcare
Of course, one does not necessarily need to be a healthcare professional to work in healthcare. Hospitals employ food service workers, custodians, data analysts, HR staff, and many other professionals. Even so, Indeed data show that demand for these types of roles is falling relative to demand for healthcare-specific roles. As of January 2026, non-healthcare-oriented roles made up about 35% of job postings by healthcare companies, down from 43% at the start of 2018.
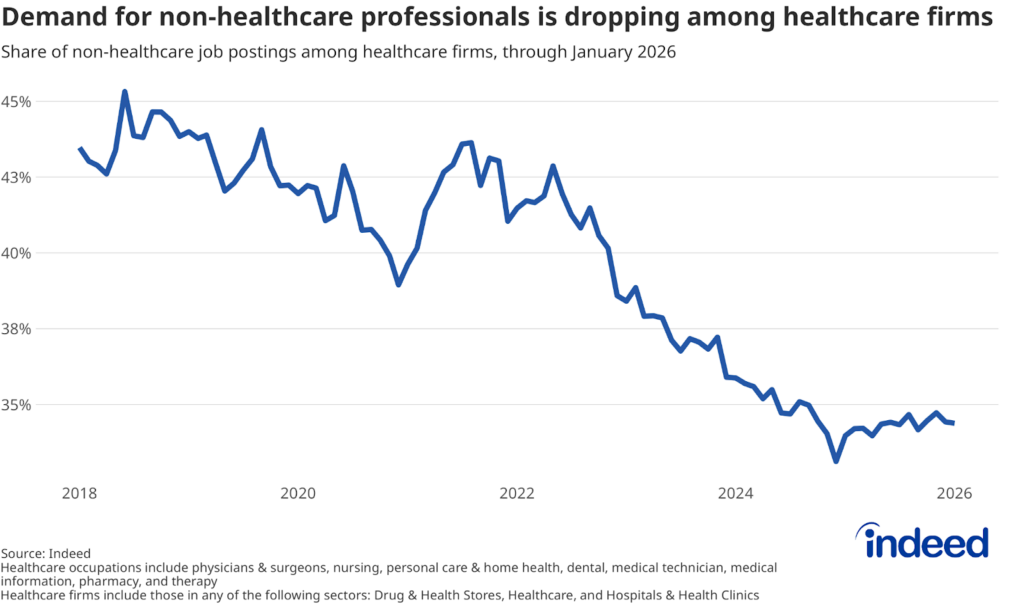
These recent trends suggest that healthcare’s continued ability to absorb workers displaced from other industries may increasingly rely on efforts to train them for healthcare-oriented roles.
Concentrated hiring in healthcare may threaten job quality
Even for those who can switch into the healthcare and social assistance subsector (or already work in it), increasing concentration within the healthcare system may threaten job availability in the long run. Indeed data indicates that more healthcare roles in Q4 2025 were in companies focused solely on healthcare than in Q4 2022. For example, it became less common to see a nursing job posted by a school or a manufacturing company, and more common to see one posted by a hospital or a doctor’s office. In Q4 2022, just under 20% of all healthcare jobs were posted by firms where 91-100% of all their job postings were for healthcare roles. By Q4 2025, this had increased to almost 26%, meaning a growing share of healthcare jobs are being posted by firms that focus almost entirely on healthcare.
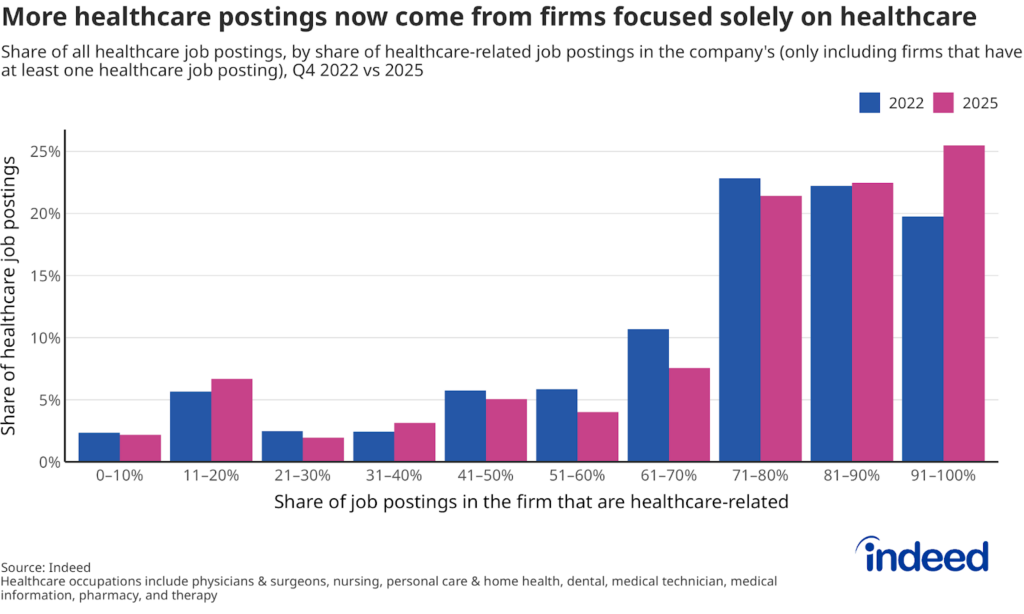
The shift in postings toward highly specialized healthcare employers in our data could be an indication that healthcare workers are increasingly dependent on a smaller set of dominant health systems for jobs.
That increasing concentration of jobs could also be impacting how both new and long-time healthcare workers view their industry. Recent research from Glassdoor shows healthcare employers receive slightly lower Glassdoor ratings than other sectors — especially on management and pay — though workers in healthcare report stronger confidence in their companies’ future. Workers transitioning from non-healthcare into healthcare companies report mixed reviews; typical review scores fell slightly for those who transitioned as a healthcare professional at a healthcare company, while reviews for those who switched to a healthcare company in a non-healthcare role rose somewhat.
As the healthcare sector continues to grow, the conditions within that sector matter more than ever. If increasing employer concentration is contributing to weaker pay and management experiences, the sector’s role as a labor market stabilizer may come with hidden costs for workers.
Conclusion
Healthcare and social assistance have emerged as a critical pillar of the US labor market, adding hundreds of thousands of jobs over the past few years, even as hiring has softened across much of the broader economy.
Still, the subsector’s ability to serve as a safety valve for displaced workers is limited. High licensing requirements in several healthcare and social assistance occupations create steep barriers for those looking to transition from other, slowing industries. At the same time, increasing consolidation within healthcare systems risks compressing wages and reducing employer competition.
The healthcare and social assistance subsector will likely continue to grow. But whether that growth translates into broad-based opportunity for workers across the economy will depend on how policymakers, employers, and training programs address the barriers that stand between a slowing labor market and one of its last remaining anchors.
Methodology
For the purposes of this post, job postings for healthcare occupations refer to job titles classified as one of the following occupational categories according to Indeed’s taxonomy structure: physicians & surgeons, nursing, personal care and home health, dental, medical technician, medical information, therapy, pharmacy. When referring to the healthcare and social assistance sector, we additionally include occupations in childcare and community and social service.
Licensing requirements are grouped into two categories: “healthcare-related” and “other.” If a job posting lists at least one healthcare-related license requirement, even alongside non‑healthcare licenses, it is classified under the “healthcare license” category. Healthcare licenses span a broad range, including but not limited to nursing, mental health, child development, and radiology.
Healthcare companies are defined as firms belonging to any of the following sectors: Drug & Health Stores, Healthcare, and Hospitals & Health Clinics. While most healthcare firms can be reliably classified into these categories, some smaller firms may be excluded due to classification limitations.
The number of job postings on Indeed.com, whether related to paid or unpaid job solicitations, is not indicative of the potential revenue or earnings of Indeed, which comprises a significant percentage of the HR Technology segment of its parent company, Recruit Holdings Co., Ltd. Job posting numbers are provided for information purposes only and should not be viewed as an indicator of the performance of Indeed or Recruit. Please refer to the Recruit Holdings investor relations website and regulatory filings in Japan for more detailed information on revenue generation by Recruit’s HR Technology segment.


